Understanding Endometriosis: A Perspective from a Gynecologist
Endometriosis is a common and often painful condition that affects about 10% of women of reproductive age. It occurs when tissue similar to the lining of the uterus (endometrium) grows outside the uterus, usually on the ovaries, fallopian tubes, pelvic wall, or other organs. This tissue responds to hormonal changes and bleeds during menstrual cycles, but unlike normal endometrium, it has no way to exit the body. This can cause inflammation, scarring, adhesions, cysts, and chronic pain12.
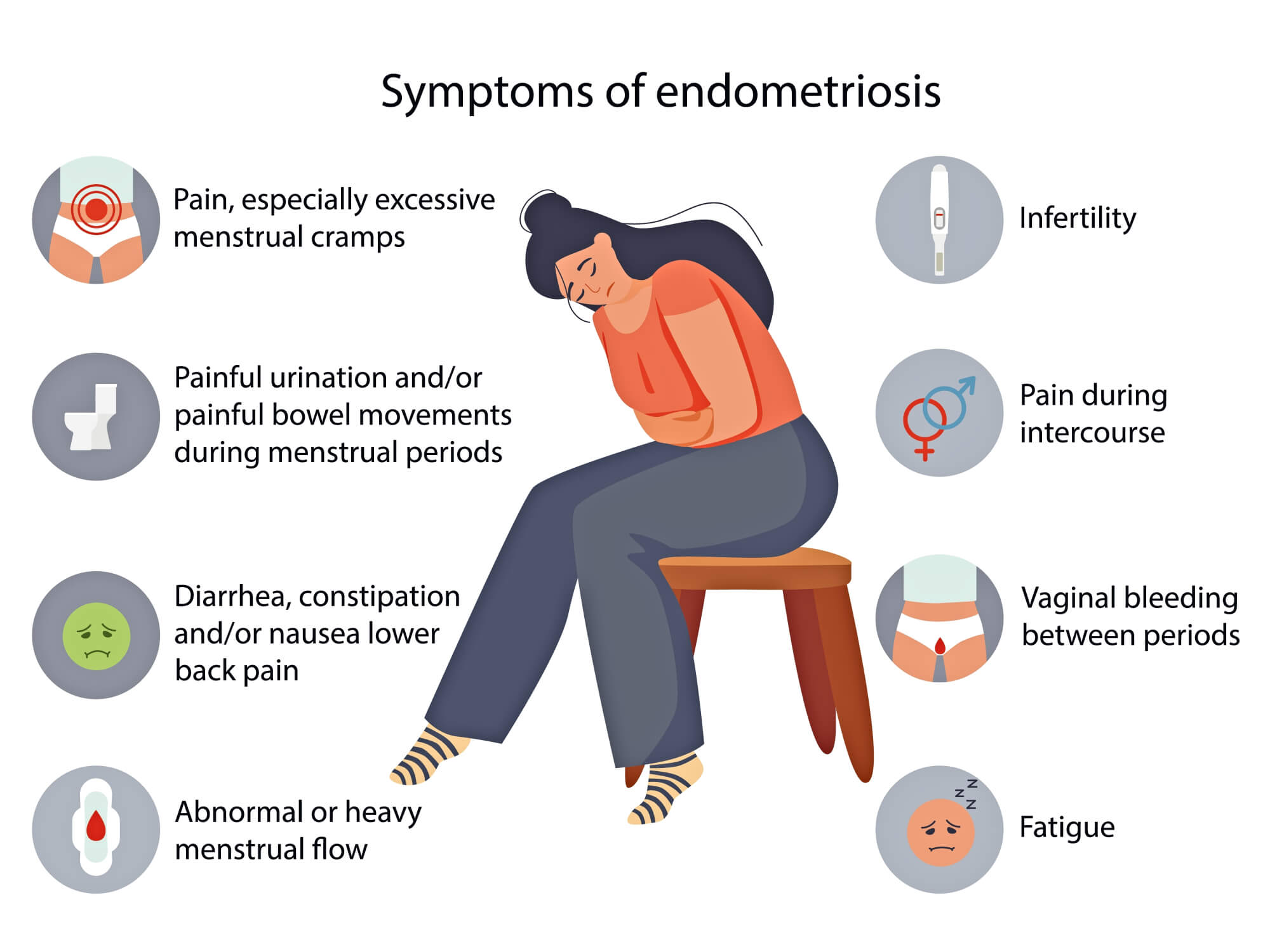
As a gynecologist, I see many women who suffer from endometriosis and its impact on their quality of life. Endometriosis can cause various symptoms, such as:
Severe pelvic pain, especially during periods, ovulation, sex, bowel movements, or urination
Heavy or irregular bleeding during periods or between periods
Infertility or difficulty conceiving
Fatigue, nausea, bloating, or mood changes
The exact cause of endometriosis is not known, but some possible factors include:
Retrograde menstruation: when some menstrual blood flows backward through the fallopian tubes and implants in the pelvic cavity.
Genetic predisposition: having a family history of endometriosis increases the risk of developing it.
Immune system dysfunction: having a weakened or overactive immune system may affect the ability to clear endometrial cells from abnormal sites.
Hormonal imbalance: having excess estrogen or low progesterone may stimulate the growth of endometrial tissue outside the uterus.
Environmental exposure: having contact with certain chemicals or toxins may alter hormonal or immune function and increase the risk of endometriosis.
Diagnosing endometriosis can be challenging, as there is no definitive test for it. The diagnosis is usually based on a combination of medical history, physical examination, imaging tests (such as ultrasound or MRI), and laparoscopy (a surgical procedure that allows direct visualization of the pelvic organs). Laparoscopy is also used to classify endometriosis into four stages according to its location, extent, and severity.
Treating endometriosis can also be difficult, as there is no cure for it. The treatment options depend on several factors, such as the age, symptoms, severity, fertility goals, and preferences of the patient. The main goals of treatment are to relieve pain, reduce inflammation, prevent progression, and preserve or restore fertility. The treatment options include:
Medications: such as painkillers (e.g., ibuprofen), hormonal contraceptives (e.g., pills, patches, rings), progestins (e.g., injections, implants), gonadotropin-releasing hormone (GnRH) agonists or antagonists (e.g., injections), aromatase inhibitors (e.g., pills), or immunomodulators (e.g., pills). These drugs work by reducing inflammation, suppressing ovulation, shrinking endometrial tissue, blocking estrogen production, or modulating immune response.
Surgery: such as laparoscopy or laparotomy (a larger incision). These procedures involve removing or destroying endometrial tissue from abnormal sites using various techniques (e.g., excision, ablation, cauterization). Surgery can provide more effective and long-lasting pain relief and improve fertility outcomes than medications alone. However, surgery also carries some risks and complications (e.g., infection, bleeding, damage to organs) and does not prevent recurrence of endometriosis.
Complementary therapies: such as acupuncture, herbal medicine, dietary changes, exercise, stress management, or counseling. These therapies may help improve physical and mental well-being and cope with the symptoms and emotional impact of endometriosis. However, there is limited evidence to support their effectiveness and safety for endometriosis